Reprinted with permission from Managed industry, June 1996
The health care industry, in a constant state of evolution and change, has been described as having four stages, each marked by increasing levels of managed care penetration and related market characteristics. Reflecting on these four stages can help health care executives to understand the dynamics of the market in which they operate and to design strategies for competing effectively in each stage. If you are out of sync with the market (for example, to use Stage 2 thinking when in fact the market is in Stage 3), you always will be playing catch-up in this rapidly evolving market.
To best apply this concept of market evolution, health care executives must reflect on where they are now and where they are going. Most major markets ultimately will reach the most advanced stage of managed care (Stage 4), in which providers and plans are fully integrated and operating to some degree under global capitation. With this writing on the wall, it is not difficult to develop long-term strategies for success under managed care.
Defining value in the managed care setting
As managed care penetration has increased across the United States, health care markets have behaved like many commodity markets, in which competitive pressures, combined with the efficient flow of information, drive prices to record-low levels. Providers and plans subject to these pressures ultimately stabilize profit margins and recognize their limits in competing further on price without suffering significant financial loss. Proof that health care markets are behaving in this manner today is found in a Foster Higgins study showing that among cost, quality, access and satisfaction, employers and other purchasers of care still regard price as the most significant determinant in their selection of a provider and a plan.
When price-based competition no longer can be pursued because of equalization in prices and profit margins, competitive organizations turn to value strategies to differentiate themselves in the market. The simple equation V= Q/P provides some perspective on the concept of value (V), defining it as the relationship of quality (Q) to price (P). The higher the price relative to perceived quality, the lower the perceived value. Consequently, organizations that operate in markets under significant, ongoing price pressure either will outsource to add cost-effective programs or will look to internal core competencies that build quality, both of which will add value to the organization’s services without raising the overall cost of goods.
Adding value through personal health management
Whether outsourced to a national supplier or created from internal resources, telephone-based personal health management (PHM) programs increasingly are recognized as effective strategies for controlling costs while improving access to health care services, thereby raising member satisfaction. The recent emergence of tile PHM movement occurred when health care organizations began to realize that these programs could contain costs and boost satisfaction simultaneously. How do they improve member satisfaction? By simply expanding access to health information through a combination of audio-library services and nurse-staffed phone lines. The popularity of these programs in Stage 4 markets is a testament to the potential for adding value without adding cost.
These programs consist of a variety of services, often based in a medical call center, designed to manage health care demand by triaging medical inquiries, supporting health and drug education, proactively managing the needs of high-risk members and generally assisting members in the responsible use of limited resources. When implemented correctly, they:
- Reduce health care expenditures by ensuring appropriate use of resources.
- Improve access to health care resources through a combination of interactive programs and services.
- Improve satisfaction through responsiveness to member needs and concerns.
- Support total quality management initiatives by enhancing health status and documenting outcomes.
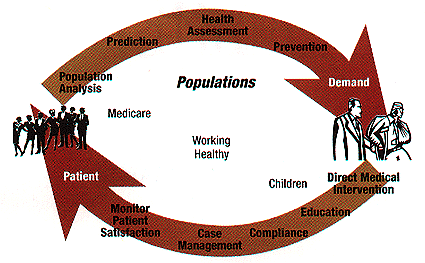
Defined in the broadest sense, PHM programs support the continuum of care from assessment to direct medical intervention to outcome measurement (as outlined in figure 2).
Personal health management and cost control
Most providers and plans establish comprehensive medical call centers to support some or all of the components that precede or follow any direct medical intervention. This trend has given rise to the growing interest in disease management programs, which apply the rigor of proactive health management to a disease state that already has been diagnosed and for which a standardized treatment regimen has been established. Organizations that successfully employ these aggressive tactics recognize the impact of “Pareto’s principle,” which says that 20% of any population will consume 80% of the resources. By applying the proper techniques to these high utilizers, providers and plans can tackle quickly the problem of adverse selection and related influence on costs.
The greatest impact of PHM generally wilt be seen in more effective use of the physician’s office and emergency room. Roughly 40% of visits to these sites are unnecessary (according to various estimates by the General Accounting Office and other sources), so medical call centers applying the concept of health management find that more effective treatment often is available from outpatient clinics or simple self-care. Members receive advice on how to treat themselves, and they report high levels of satisfaction when they learn they need not wait for medical. Intervention to treat a common injury or health problem.
Of particular interest to health plans is the impact of health management programs on the cost of adjudicating certain medical claims. At CIGNA industry of Arizona, a medical call center-fields calls from members across the state in order to authorize all uses of emergency services. Members are provided an authorization number (a unique number generated by the call center) indicating whether payment for the visit will be approved or denied. Members who do present that number in an emergency room know from the moment they arrive whether the visit will be covered or not. With no “gray area” preceding or following the encounter, CIGNA receives fewer complaints and contested claims. This CIGNA region, ranking among the company’s top in profitability and member satisfaction, received full three-year accreditation from the National Committee for Quality Assurance on the strength of its various health management programs.
Personal health management as a member benefit
A recent Consumer Reports study found that dissatisfaction with health plans often is correlated with chronic health problems, as additional stress and psychosocial problems cause frustration for members with these conditions. Although these members are not likely to receive better attention or advice elsewhere, they often “vote with their feet” every year, looking for a plan more sensitive to their special needs. Introduction of PHM initiatives can improve their satisfaction dramatically, ensuring that they will not take their premiums to a new plan the following year. For this reason, a PHM program ideally is introduced as a member benefit, with materials devoted to discussing how the program will improve access and member satisfaction. While launching the program involves start-up costs, the investment is justified on the grounds that it yields more effective utilization and helps retain members who otherwise might have changed health plans.
Many providers and plans find it easiest and quickest to outsource call center services and other health management programs w that they can concentrate on their mission as a provider or integrator of medical services. Others find they must be able as “soon as possible to compete within the rapidly shifting dynamics of their market or to comply with new contracts they have signed. That the PHM movement is under way was given solid confirmation by a recent Center for Corporate Health study that found that 25% of ail health plans will launch a medical call center this year to support their own PHM initiatives.
While health plans and provider groups are focused on re-engineering for managed care, the argument for including PHM as an element within the information systems infrastructure appears well established. Personal health management adds value by controlling costs and improving quality, and it extends organizations’ ability to grow by providing more efficient access to limited resources.
by Ian R. Lazarus Reprinted with permission of the author. Mr. Lazarus may be contacted at irl@creato.com.