Before they can realize their true potential, EMRs must be the carefully defined product of a multidisciplinary effort
By Ian R. Lazarus, FACHE and James M. Gabler, MS
If an electronic medical record is indeed “the holy grail” of medicine, then it has proven itself as elusive as the legendary original. Discussed in theory for decades and attempted through iterative product releases from capable vendors, the electronic medical record (EMR) remains an ideal without a universally-accepted prototype. Still, the benefits from this technology platform are so compelling that providers and their suppliers continue to commit time and energy toward it. The anticipation and effort -from the perspective of those that want it and need it – could be compared to landing a man on the moon. What most organizations lack, however, is an effective plan to accomplish the goal. Impending regulation to standardize, protect and safeguard patient data will quickly change things.
To undertake such an initiative will inevitably effect many stakeholders in the organization, and many decisions made today on IT applications must be approached with consideration of how it will impact the eventuality of an electronic medical record system. Indeed, an effective plan for deployment is as important to the success of an EMR initiative as having capable software to use once deployment is complete. The purpose of this article is to set forth some basic guidelines for organizations that are committed to an EMR and do not want to be dependent on proprietary vendor-related initiatives.
Taxing Syntax. The development of an electronic medical record has so much history that any discussion of it must be preceded by some basic groundrules. First, the definition must be established, and the terminology describing it must be consolidated. For example, some have arrived at the concept of an EMR from a computerized patient record (CPR) and some have moved from here to discussion of an electronic health record (EHR). These are all intended to describe the same underlying technology but are simply attempts to find a description (and acronym) that is suitably holistic and comprehensive. Defining the initiative and the basic functions of the desired system must be established first before moving forward with discussion on its merits.
Second, the anticipated benefits must be clearly articulated and understood, with a further segmentation of those that will be experienced immediately after implementation and those that will require organizational changes in behavior. Calculations of return on investment might rely upon assumptions provided by the vendor for the former, but the latter requires the organization to test its resolve to achieve the possibilities, and more conservative estimates of ROI are needed. For example, EMRs are expected to confer the following benefits:
Benefits of a effective EMR system
- Improved workflow
- Reduced medication errors
- Prompt, error-free communication
- Better bedside decisions
- Enhanced patient education
- Improved continuity of care
- Reduced morbidity and mortality
- Improved reimbursement, fewer denials
- Reduced malpractice premiums
- Better outcomes data and reporting
- Improved patient/provider satisfaction
- Effective regulatory compliance
- Easier achievement of accreditation
- Improved competitive advantage
Many of these benefits defy accurate quantification. An IDS recently approved a electronic patient medication system with a pricetag of $40 million after only cursory consideration of ROI. The system would take information traditionally available to pharmacists and present the data on handheld devices to physicians for use during treatment. After struggling with attempts to project return-on-investment using many of the anticipated benefits listed above, the expenditure was approved on the strength of the argument that it would improve competitive position and relationships with the medical community, a key stakeholder in the institution’s success. Indeed, ROIs may be of little benefit as EMRs attempt to “prove themselves” in the market, but they will become essential in understanding the broad potential impact of the product and, as more systems become available, in distinguishing the strength of one solution against another.
Finally, the organization should establish a multidisciplinary team to identify the various dependencies for effective implementation of the EMR, and the desired attributes from the system, with a distinction between the “nice to have” features and the “must do” capabilities. Although “management by committee” can have its drawbacks, the alternative places far too much responsibility on the IT department to select a system for use by all.
EMR Theory. Fortunately, IT theorists have given us a useful framework for the purposes of defining the ideal EMR. Gartner Research has both defined the attributes of an ideal EMR and the various iterations anticipated in the evolution of the ideal.
Their definition (using the term “Computer-based patient record system,” or CPR) describes a “system that contains patient-centric, electronically maintained information about an individual’s health status and care. It focuses on tasks directly related to patient care, unlike other healthcare information systems that support providers’ and payers’ operational processes. The (system) completely replaces the paper medical chart and thus must meet all clinical, legal and administrative requirements.”
GartnerGroup’s attributes of an Electronic Medical Record (EMR) System
- Provide clinical documentation and capture data
- Display data effectively to support decision making
- Storage which is compliant with regulation and easily retrieved
- Management of clinical tasks and protocols
- Decision support from simple alerts to algorithms and artificial intelligence engines
- Links to medical references and relevant content databases
- Security to protect and safeguard confidential data
- Integration with subsystems that feed and accept data
Source: Gartner Research
In setting forth the definition of an EMR and its various components and capabilities, GartnerGroup acknowledges that the requirements may be met through an underlying architecture or framework and not necessarily through the implementation of a single product.
Summary of EMR generations
- First generation: The Collector – simple systems that provide a site-specific solution for the need to access clinical data which is imported through scanning or other forms of aggregation
- Second generation: The Documentor – basic systems that clinicians use at the point of care to adequately document rather than merely access clinical data
- Third generation: The Helper – Systems that include episodic and encounter data and use decision support tools to assist clinicians, functional in at the minimum both ambulatory and inpatient settings
- Fourth generation: The Partner – Advanced systems that provide more decision support capabilities and that are operational and accessible across the continuum of care, and providing sufficient credibility as to become the patient’s legal medical record
- Fifth generation: The Mentor – Complex and fully integrated systems that include all previous capabilities and that are a main source of decision support in guiding patient care for both clinicians and consumers
Source: Gartner Research
Window Shopping. Although models set forth by research organizations help provide a framework for understanding the evolution and capabilities of an EMR, attempts to simplify the selection process remain confounded by the different approaches taken by the vendors at delivering the desired capability. Healthcare organizations accordingly face an array of options and it becomes difficult to compare these in a traditional cost justification exercise because of the long term implications of each decision. The most significant of these decisions today is whether to license the technology or to accept an “ASP” (Application Service Provider) solution, which is comparable to leasing the application and accessing it over the web. Software vendors are moving rapidly to add ASP-options to their product suites as the revenue model is more attractive to them than the traditional licensing of software applications.
“Its very hard to do a comprehensive value analysis of an EMR, but the difficulty is not primarily a function of whether it is an ASP or not,” notes John Glaser, Ph.D. Chief Information Officer for Partners HealthCare System in Boston, MA. I think the value analysis is the most significant challenge but this is less significant than the implementation effort.” Glaser notes he is currently using value analysis to compare ASP vs. licensing options for practice management systems.
There are also emerging features from EMR releases that command immediate attention. To be fair, these features promise to deliver significant, immediate value to the organization, and arrive with such fanfare that they weigh heavily in the customer’s evaluation of overall system merits. A typical example of this is the process of physician order entry (“POE”), a process that drives 80 percent of the care delivery costs in healthcare organizations. A capable order entry system will include several integrated functions: order processing, capture, management, communication, billing and workflow support. Because this process is central to the care provided to the patient, it can also generate data to support efforts to enhance quality and contain costs. A capable POE is even expected to reduce pharmacy administration costs since embedded decision rules will avoid prescribing errors, once of the most common problems in medical care. POE capability is one of the three medical error reduction initiatives supported by The Leapfrog Group.
Finally, another key consideration is the breadth of initial deployment. Most IT departments recognize the challenge of deploying EMRs throughout the organization, yet they concurrently resist the notion of supporting an array of different applications to satisfy the needs of each department. Vendors, for their part, have an incentive to reach into as many departments as possible, even though an application that might serve the needs of one department or function is a poor fit for another. Vendors also wish to migrate users onto one common application to reduce their costs to maintain and upgrade application platforms.
“Best of Breed” vs. “Best of Fit.” The evolution of EMRs to date has given rise to another implementation issue facing healthcare organizations. While the concept of “Best of Breed” has been an effective decision criteria to guide procurement decisions in the past, the broad reach of an EMR, coupled with limited vendor offerings, has given pause to this approach since no final solution exists that is deserving of such a distinction. Instead, IT executives have moved their focus, by default, to “Best of Fit.” This, in turn, has inevitably resulted in heterogeneous solutions across the enterprise, leading to integration challenges. All of this might cause the most seasoned IT executive to take up stress reduction therapy.
Against this backdrop there are the efforts of some organizations to lend sanity to the challenge posed by EMRs. One vendor, MediServe Information Systems, announced this year their sponsorship of an “Info Tech Study” to identify the most critical applications sought by caregivers and the departments most likely to benefit from EMRs. Two co-sponsors, the American Health Information Management Association (AHIMA) and the American Medical Rehabilitation Providers Association (AMRPA) have joined MediServe to help support the initiative. Creato, a biotechnology consulting firm, is conducting the Study (those interested in participating may visit www.creative-healthcare.com to enroll). The collaborative effort hopes to reach out to clinicians and IT executives in further identifying the implementation issues and critical features needed from an EMR initiative. “The vendors need to listen to the market,” notes Bruce Mortensen, President of MediServe. “And some of challenges faced by the industry today is because we haven’t listened enough.”
MediServe hopes to challenge conventional wisdom that an enterprise-wide system can deliver on its promise of convenience and cost effective integration of data. “We have seen just how difficult it can be to address the multiple requirements of very different ancillary departments,” notes Mortensen. “We believe the industry will ultimately conclude that independent systems, once linked, will represent the best of both worlds.” MediServe specializes in EMR systems for clinical ancillary departments and finds many clients migrating their MediLinks platform to one department at a time, coming even closer to a true enterprise-wide EMR.
Data Depots. The emerging framework for EMR deployments has resulted in the evolution of a coordinated network of smaller databases that focus on specific roles within the application as a whole. To make an analogy, credit card issuers combine charges into one database for monthly billing, but they are highly dependent for charge capture on a multitude of disparate applications around the world in every participating merchant. The credit card number is the coordinating “tag” that creates synergy from this collection of disparate systems. The coordinating tag must be issued and controlled by the consolidating entity, adding an external coordination role to traditional database responsibilities (see figure below).
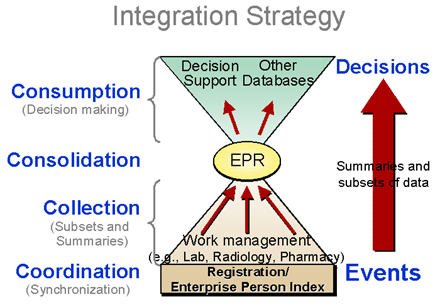
In a managed care organization, the EMR consolidates information about a patient collected through the care processes and enables the decision-maker (physicians and nurses) to have a more complete view of the patient’s medical condition. The various types of information are captured in disparate work management applications unique to the activities of each ancillary role. In this respect the independent EMRs operate as traditional database systems, except for the required external synchronization. Within a centralized database, coordination is automatically accomplished by each database entry having a unique record ID: the internal coordinating tag described above. When data comes from multiple sources as it does in the managed care entity, the coordinating tag must be externally assigned and controlled. This process allows a great deal of freedom in collecting and allowing patient information to flow to the EMR where it can be effectively managed and augmented as necessary throughout the continuum of care.
EMR Endpoint. While the industry waits for reliable EMR solutions, it is incumbent on each managed care organization to understand the benefits, capabilities and limitations of current and future products. To be sure, there will be sacrifices made and tradeoffs required for most currently available solutions, but the key to enjoying the benefits will be to have an endpoint in mind. That endpoint will necessarily include a system that delivers better care at a lower cost.
In the final analysis, it’s also critical to remember that technology alone will not deliver the benefits they make possible. Sensible planning to achieve synergies between systems is the first step. Changing behavior to tap the potential of the technology is the next step. Although beyond the scope of this initial review into EMR capabilities, the combination of suitable, integrated technology with a commitment to tap its potential holistically will ultimately deliver the best value to the organization and its customers.
Ian R. Lazarus is managing partner of (Creato), a provider of process improvement methodologies, and James M. Gabler is Research Director for (Gartner, Inc).